Periodontal (Gum) Disease
The two most common forms of dental disease, caries (tooth decay) and periodontal disease (gum disease) are caused by the presence of bacterial communities in dental plaque, which is a sticky film that is constantly accumulating in the mouth. While in the case of tooth decay the acidic products of the plaque bacteria progressively erode tooth structure, in gum disease an inflammatory response is provoked in the periodontal tissues that surround and support the teeth. If left untreated, periodontal disease can lead to gingival pocket formation, gum recession and diminishing alveolar bone with the eventual loosening and loss of teeth.
According to the Centers for Disease Control and Prevention (CDC), one out of every two adults aged 30 and over in the United States is affected by periodontal disease. Furthermore, that number increases to over 70% for individuals 65 and older. Since gum disease is the main cause of tooth loss in adults and there is an increasing association with systemic diseases such as heart disease, stroke, diabetes, respiratory problems and adverse pregnancy outcomes, periodontal disease represents a serious public health concern.
Although inadequate oral hygiene practices, infrequent dental checkups and few if any professional teeth cleanings are the main reasons for the development of gum disease, there are other factors that can contribute to the risk. An individual may be predisposed to periodontal disease because of genetic factors, smoking and tobacco use, harmful oral habits, misaligned teeth, poor nutrition, and stress as well as the fluctuating hormones in pregnancy. Diseases such as diabetes, rheumatoid arthritis and HIV infection can also increase the risk and severity of periodontal disease. Additionally, certain medications for the therapeutic treatment of systemic disease can lay the groundwork for periodontal problems by producing side effects such as dry mouth (xerostomia) or causing the gums to enlarge.
What are the signs and symptoms of gum disease?
Since much of the course of periodontal disease is not painful, there may be little awareness by an affected individual that a condition, which is harmful to oral health as well as one that is linked to larger systemic problems, is present.
Some of the signs and symptoms of gum disease to be aware of include the following:
- Inflamed and red gums
- Bleeding when brushing or flossing
- Receding gums and exposed root surfaces of the teeth
- Sensitivity to hot or cold temperatures
- Bad breath or a bad taste in the mouth
- Teeth that feel loose
- The development of new spaces between the teeth or a change in the bite
- Change in the fit of existing partial dentures
- Discharge around the teeth and gums
- Sharp or dull pain when biting down or chewing food
While gum disease is a progressive condition, if treated early in its onset it can be reversed to restore oral health. At more advanced stages, the disease can be managed to halt its progression and prevent the most severe consequences.
The earliest stage of gum disease is known as gingivitis, which is caused by the buildup of dental plaque at the gumline. Gingivitis is extremely common and is typically associated with bleeding when brushing or flossing. With gingivitis there is no evidence of bone loss or significant periodontal pockets between the teeth and gums. Gingivitis can be successfully treated and reversed with a series of professional dental cleanings and an improved regimen of oral hygiene at home.
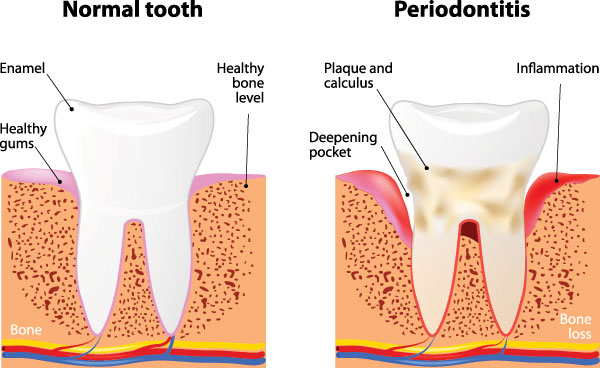
If gingivitis is allowed to progress, it can advance to the next stage, which is known as periodontitis. When periodontitis is present, the tissue damage extends beyond the gums to include the loss of the collagen attachment of the tooth to the surrounding bone, the development of deep periodontal pockets and the loss of supporting alveolar bone. In this stage the connective tissue and bone that hold the teeth in place begin to break down. Without proper treatment, periodontitis will progress from a mild to moderate loss of supporting tissue to the complete destruction of the alveolar bone around the teeth. As periodontal treatment advances, more extensive procedures are required to halt its progression. The dentist may recommend a series of deeper cleanings involving root planing and scaling, surgical procedures to reduce pocket depth, bone or tissue grafts, laser dentistry procedures, or antimicrobial medications.
By far, the best approach to care is the prevention of periodontal disease. By maintaining an effective regimen of brushing and flossing at home, following a healthy lifestyle and seeing the dentist for routine checkups and professional dental cleanings, gum disease and its consequences are largely preventable.

